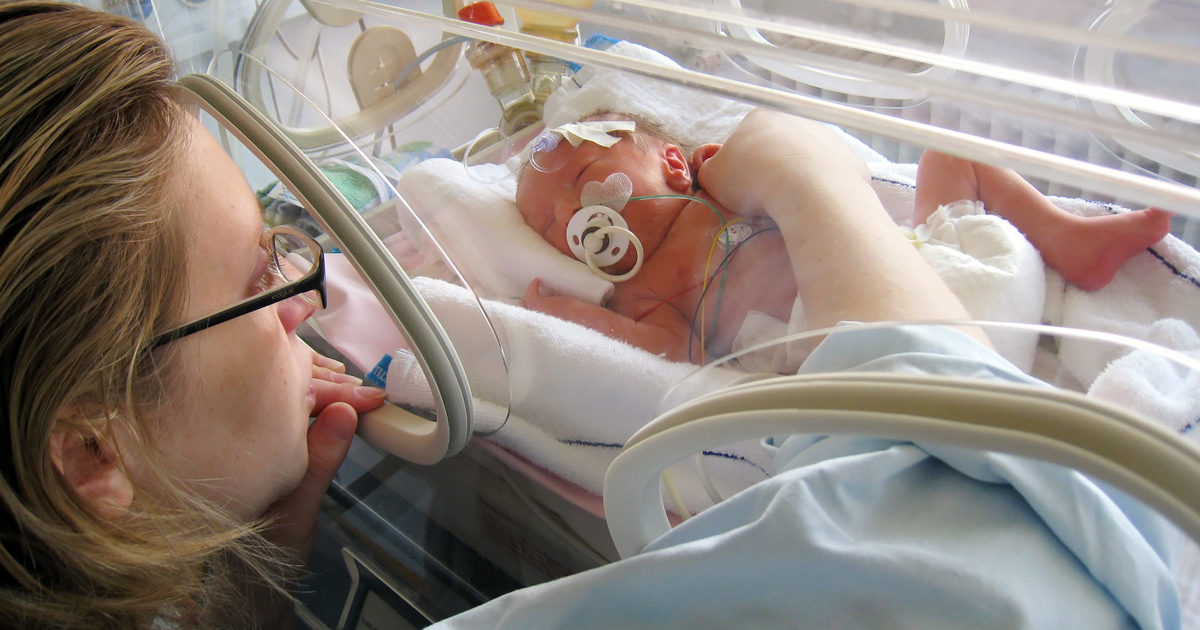
The impact of Coronavirus Disease 2019 (COVID-19) is vast and unbiased. Once-in-a-lifetime events are being marred by the disease itself and the restrictions that come with it. Birth is no exception. Yet, we expect the same, some might argue better, quality of care from our doctors and nurses. An initial shortage of personal protective equipment (PPE) was one of the most publicized concerns during the current crisis, but for those working in the NICU it’s the tip of the iceberg for COVID-centered care.
Adapting to a new care model
There has been a rapid deployment of care protocols to manage infants born to mothers with suspected or confirmed COVID-19, starting with pre-screening measures for pregnant women and their one allotted partner/visitor. In the NICU, where newborns are already in need of specialized care, the changes caused by COVID-19 can be felt even more acutely. Neonatal resuscitation, post-delivery care, parental visits, and support of breastfeeding have all been impacted. The number of providers attending deliveries must be minimized to reduce the spread of COVID-19 and to prevent loss of critical providers due to exposure and mandated quarantine.
Isolating exposed infants is equally important but is complex due to the need to keep newborns six feet away from their mothers and to make sure the mothers are using PPE appropriately. While the safety of breastfeeding has been called into question, breast milk has been deemed not only safe but still very beneficial to a NICU (or non-NICU) baby. Proper handwashing, use of a mask, and a clean breast pump are all essential steps for reducing exposure from a COVID-19 positive mother.
Whether COVID- 19 can be vertically transmitted (passed from the mother to her fetus in-utero) is unknown. Our health care teams are contributing to research to identify neonatal symptoms for COVID-19 term so as to better identify neonates who need special care and long-term follow-up. The Centers for Disease Control and Prevention (CDC) lists these possible signs of COVID-19 for newborns: fever, lethargy, rhinorrhea, cough, tachypnea, increased work of breathing, vomiting, diarrhea, and feeding intolerance or decreased intake. However, many of these signs are common among NICU babies. This puts additional burden on the care team as they must take all these factors into account, in addition to the acute issues they monitor on a daily basis.
Impact beyond clinical
The emotional toll is hard. Changes in parental visitation and separation of COVID-19 exposed infants from their parents creates stress, anger, and sadness in both the providers and family members. Jena Petry, a MEDNAX NNP-BC, said it best – “The day-to-day impact of COVID-19 is heartbreaking.” Implementation of visitor limitations, intended to protect patients and staff, often means a mother may not have anyone there to support her when hearing difficult and frightening news. Clinicians may experience separation from their immediate families as well. Because of potential exposure to the virus, clinicians often choose to stay away from their families to protect them from exposure.
A message from MEDNAX
During the COVID-19 crisis, our patients and their families remain our priority. To ensure access to care while minimizing potential COVID-19 exposure, we’re working closely with internal experts, hospital partners, and health care authorities at the national, state, and county levels to implement and adapt care protocols in real time. We have used innovative methods to care for patients and families and will continue to work to improve upon this delivery of care. Despite this global pandemic, we’re also focused on the future; we’re working collaboratively across the continuum of care to better understand ─ and reduce ─ the impact of COVID-19 on the patients we serve.